Screening for Breast Cancer
State of the art care, or a harmful waste of resources? It depends on who you ask!
In my previous post, I discussed the underlying premise of screening for disease, as summarized in the following quote.
The object of screening for disease is to discover those among the apparently well who are in fact suffering from disease.
In theory… screening is an admirable method of combating disease, since it should help detect it in its early stages and enable it to be treated adequately before it obtains a firm hold on the community.
In practice, there are snags.
In this post and the next, I’ll look specifically at screening for breast cancer, using mammography.
Breast cancer starts out small and then grows. The hope is that mammography will detect a breast lesion visually (using x-rays) before it becomes a palpable lump. It deserves emphasis that:
Breast screening does not PREVENT you from getting breast cancer.1 Any lesion detected on the mammogram was present for a while before the mammogram was done.
Mammography is also fallible, in that small cancers can be present but too small to be seen on the mammogram. Having a negative screening mammogram is no guarantee that you don’t have breast cancer.
Mammography done to investigate a palpable lump is DIAGNOSTIC mammography, NOT screening mammography. They are different!2
Based on favorable randomized trials back in the 60’s and 70’s, mammographic screening for breast cancer became widespread in the 80’s and 90’s, continuing to the present day.
Early marketing campaigns were fairly aggressive, including this example from the American Cancer Society claiming that “If you haven’t had a mammogram, you need more than your breasts examined.”

More recent marketing strategies are a bit more subtle (and less insulting), but still imply that by NOT having a mammogram you are somehow endangering your health.

Other ads rely heavily on statistics:
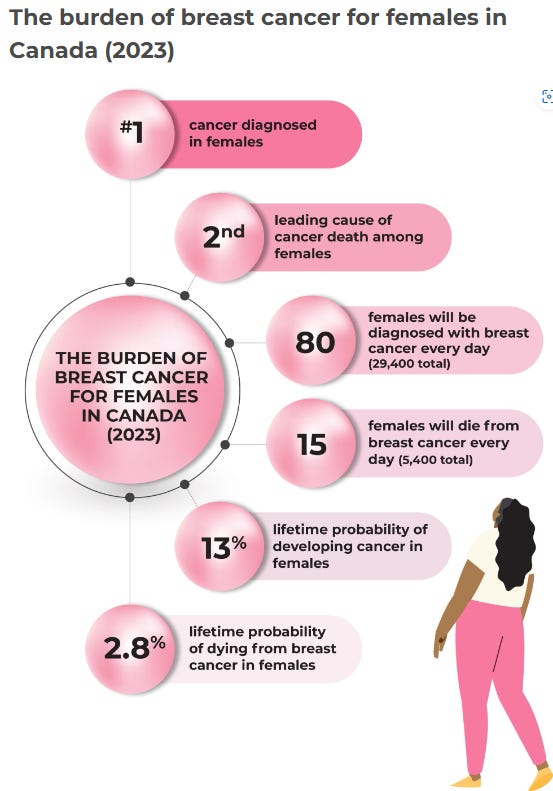
Note that the statistics are presented to be as alarming as possible3:
Sure, 13% of women will be diagnosed with breast cancer in their lifetime, but 87% won’t.
There are dozens of different types of cancer, with breast cancer making up only 25% of the total, so ¾ of cancers in women are NOT breast cancer.
In declaring that breast cancer is #1, this graphic (and most statistics) ignore skin cancers, which are extremely common but generally less fatal (other than melanoma). Any type of cancer could be #1, if you exclude the ones that are more common.
There will be an estimated 40,800 cancer deaths in women in Canada in 2024, of which 9,800 will be lung cancer and 5,400 breast cancer. So, it’s true that breast cancer is the second leading cause of cancer death in women, but 87% of cancer deaths are caused by some other type of cancer.
There are lots of ways to die. Cancer deaths make up only 1/4 of total deaths. When a woman dies there’s a 97.2% chance the cause of death was something other than breast cancer.
While 29,400 sounds like a lot of women to be diagnosed with breast cancer, it’s less than 0.2% of the female population older than 15, so 99.8% of adult women will NOT be diagnosed with breast cancer in any given year.
Regardless of how mammography is marketed, we’re certainly diagnosing more breast cancers these days, presumably because we are finding them earlier. However, there’s a possibility that we are now finding the indolent and slow-growing breast cancers, the ones that would never have caused problems had they gone undetected (a problem known as ‘over-diagnosis’ - see previous post).
Mammogram machines have changed for the better, producing better quality images with less radiation exposure. That’s good, because repeated x-rays to any organ can theoretically cause cancer.
At the same time, breast cancer treatments have improved substantially. Fewer women are dying of breast cancer, declining from 41.7 deaths per 100,000 in 1989 to an estimated 21.8 deaths per 100,000 in 2024. It’s unclear whether that’s the result of earlier detection, better treatment, or both.
At the end of the day, there is now and always has been some controversy as to whether or not mammography screening offers a net benefit.4 That’s good thing! In any scientific endeavor, it’s healthy to question the evidence, rather than accepting that the “science is settled”. In this case, the evidence is still evolving.
To that end, a plethora of learned organizations around the world regularly review the evidence about breast cancer screening, updating their recommendations as needed. Even though they all have access to the same data, their guidelines vary, most notably in terms of the frequency of screening, the age at which screening starts, and the modalities used. None have (yet) reached the conclusion that mammography is no longer an appropriate screening modality, although the recent controversy about its lack of sensitivity in “dense breasts” has caused some to suggest that other (more expensive) breast imaging methods (i.e. MRI) may be better.
In this post, I was going to review the literature, all those guidelines, and the logic that the various organizations have used to arrive at different conclusions, but I’ve decided not to, for reasons which will become apparent as you read on.
Suffice it to say for now that the guidelines reflect value judgements, and different groups have different values.
Breast Screening in the real world
I live in Nova Scotia, where the current breast screening guidelines are fairly “middle of the road”:
for women aged 50-74 with no increased risk factors, mammography is recommended every 2 years.
Everybody else (women with any risk factors, and those aged 40-49 and 75+) is encouraged to talk to a health care provider to see if screening is right for them.
Women aged 40-49 who choose to have a screening mammogram can have a yearly mammogram, and those over the age of 75 who choose to have a screening mammogram can have a mammogram every two to three years.
In looking at the 2023 Annual Report for the Nova Scotia Breast Screening Program:
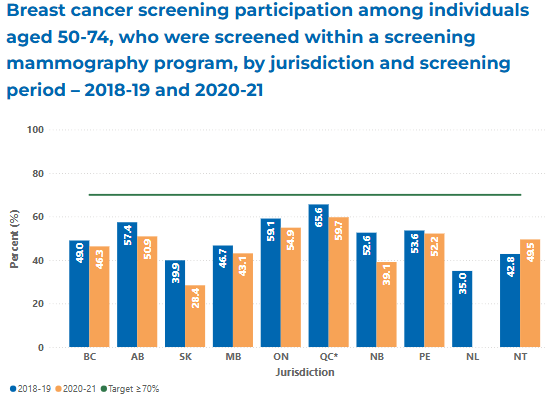
only 37.1% of eligible women aged 50–74 have actually had a mammogram in the past 30 months, well below the national target of 70%. That number has been declining since 2019.
The retention rate is also substandard, with only 20.4% returning after their first screening mammogram (target 75%), and only 57.0% returning after a subsequent screen (target 90%)5. Again, both figures have been declining.
All of which makes you wonder. If screening mammography is so obviously important, especially in the 50-74 age group, then why aren’t ALL women doing it? Do women need their heads examined? How can they be so cavalier about their health?6
Different world views
In looking at this topic, what I’ve found interesting is that it highlights the fact that there are two different perspectives on health care, sitting at opposite ends of a spectrum. I’ll call them the “medical care model” and the “public health model”. Patients get caught in the middle.
For example, in those Nova Scotia guidelines, the public health model comes through in the advice that women aged 50-74 with no increased risk factors should have mammography every 2 years. In those earlier campaigns, it was the public health model speaking, presenting mammography as something to be done, not questioned. Thinking at the abstract community level, which is how public health works, there’s clear evidence that screening mammography in certain age groups saves more lives than it harms, so why wouldn’t women want it? Ideally 100%, but they’ll aim for 70% for now.
The advice to talk to a health care provider to see if screening is right for you shifts you to the medical care model, where it’s about your personal choice. With other public health measures, like vaccinations, your decision to have a flu shot might affect the health of others (by reducing the risk of you transmitting the infection to them). By contrast, your decision NOT to have a mammogram doesn’t place anyone but you at risk. If there’s a benefit to having the mammogram, it’s your benefit. If there’s a risk of harm, it’s your harm. Your healthcare provider can help you to understand the benefits and risks, but at the end of the day the choice you make depends on what’s important to you.
So, how you regard the importance of a screening modality, like mammography, depends on your point of view.
The concept of medical care vs public health is critical. I might even go so far as to say that the misapplication of the two theoretical models explains many of the problems with our current health care system.
I’ll continue this discussion in my next post.
The breast cancer lesion has to be big enough to be seen on mammogram, so it’s not going to detect every breast cancer.
Technically, breast screening is a form of ‘secondary prevention’, in which you prevent or reduce the long-term consequences of a disease that you already have.
If you can feel a lump in your breast, you are NOT asymptomatic. Any lump needs to be diagnosed. Diagnostic mammography is usually part of the process.
I’m more of a “glass half full” sort of guy!
On the skeptical side, for example, you might want to look at 31 Days of Little-Known Facts for Breast Cancer Awareness Month or Mammography screening is harmful and should be abandoned.
80% of women don’t come back after their initial mammogram! Just under two-thirds of those that have had a couple of mammograms keep coming.
By the way, the numbers aren’t a whole lot better nationally, although they do vary from province to province.