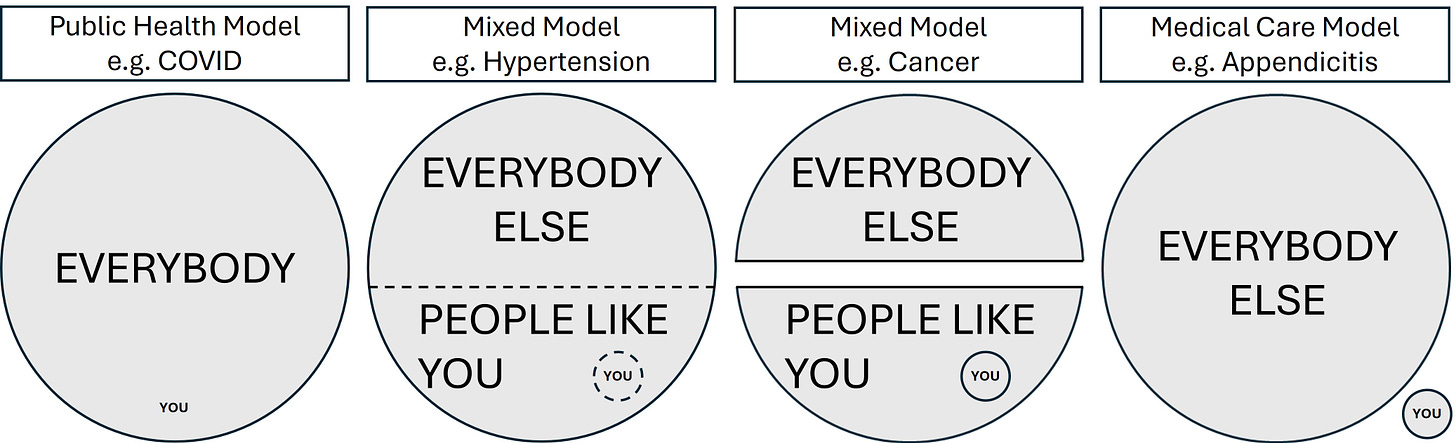
Medical care, public health, and everything in between
Making informed decisions about your health isn't always easy, especially when your advisors have different theoretical and ethical perspectives!
In my previous post, I briefly discussed breast cancer screening in the context of two different perspectives, the “medical care model” and the “public health model”.
As I see it, these sit at opposite ends of a spectrum. Patients often get caught somewhere in the middle, trying to make an informed decision about their care. The advice they receive about any intervention, including mammography, depends on which perspective is being applied, something that it’s not always easy to know.
In this post, I’ll expand on this concept, starting with a more detailed exploration of the two theoretical models and the gray zone in between. In the next post, I’ll tie it back to the mammography debate.
The medical care model
We’ll start with the medical care model, because it’s the model that most people understand best, based on their past experiences with illness and the health care system.
Medical care focuses on the diagnosis and treatment of diseases affecting you, as an individual. It tends to be reactive, addressing health concerns as they arise.
Medical interventions include things like medication, surgery, physiotherapy, occupational therapy, etc.
Medical care is based on knowledge accumulated over the centuries through the study of millions of people, including biological sciences like anatomy (structure), pathology (abnormal anatomy), physiology, and pathophysiology (abnormal function).
Your doctor and the rest of the team use all that knowledge and their past experience with patients like you to effectively diagnose your problem, inform you about the likely prognosis, present your options, and provide your care safely and effectively. Their general knowledge informs their care of you as an individual, while the experience they gain in caring for you informs and expands their body of knowledge and world view.
Your healthcare providers work for you, even when somebody else seemingly pays the bill on your behalf.1 Four main ethical principles guide their work:
AUTONOMY, reflecting the importance of freedom of choice for patients and their health care providers.
NONMALEFICENCE, best summarized by the phrase “First do no harm”, which implores them to weigh the potential risks and harms against the benefits, for everything they do.
BENEFICENCE, the injunction to act only in ways that are beneficial for the patient, providing competent care, respecting patient rights, safeguarding patient information, and treating the responsibility to the patient as paramount.
JUSTICE, which typically entails respecting individual rights and acting fairly when distributing limited resources to individual patients.
In this model, for you as a patient with a health problem, any decisions you make about your medical care are based on how your illness and treatment affect you personally. When you have appendicitis, for example, there’s you, and there’s everyone else.
You have the symptoms, your tests are abnormal, you’ll face the complications if the problem goes untreated, and you have to decide whether the benefits of an appendectomy outweigh the risks.2 It’s classic “fork in the road” decision-making. It’s immediate, it’s concrete, and it’s personal! Your problem, your values, your decision, your consequences. When it’s all over, you’ll judge whether the benefits outweighed the costs, financial and otherwise, by the results you see personally. You decide whether or not the operation was a success.
The public health model
In public health, by contrast, the focus is on the health of the population.3
Public health aims to be proactive. Classically, public health dealt with infections, where they saw good success introducing things like clean water, improved sanitation, and other infection control measures.4
Even when responding to something affecting individuals, like an infectious disease outbreak, public health deals with population-level activities, not the medical care of individual patients. For example, imagine that Mary has typhoid. Her personal medical care is delivered by the medical team, as above. The public health people may well put Mary into quarantine (to protect others), but their main focus will be figuring out who gave her typhoid and who she might give it to (Mary’s contacts, the “high risk” group).
In public health, the primary actor is most often a government agency, employing public health experts who are accountable to the public only indirectly. While some of them trained as medical doctors, others are microbiologists, epidemiologists, statisticians, sanitation engineers, etc. What they know, they learned by studying groups. Their decisions also tend to affect groups of people, especially where we can’t realistically expect individuals to make the decision that respects the “greater good”, rather than pursuing their own self-interest. For example, Typhoid Mary’s need to earn a living might mean that she won’t stay home unless she’s told to. Ditto for her colleagues at the restaurant where she cooks.
Decisions about public health measures are often based on statistics and models, looking at things like health trends, risk factors, and rates of disease. It can be an abstract and complicated process, assessing the risks and benefits for the entire population, assigning frequencies and values to the various effects, and then deciding whether the overall good outweighs the overall bad, all through the lens of societal values. Statistics are subject to bias and interpretation, and mathematical models include various assumptions which may or may not be correct. Societal values reflect averages, with much variation. The benefits and risks may occur now or in the future, they may be specific (death) or vague (feeling unwell), some will be well-documented and others unknown, and citizen concerns may seem rational or irrational.5
In some cases, it’s pretty simple. Clean drinking water, for example, likely benefits everyone and harms nobody. Fluoridation, on the other hand, is a bit more controversial; some people don’t want chemicals in their drinking water, and they’ll fight about it for years.
Immunizations, as another example, may reduce the frequency and severity of a given infectious disease in the community, but only when given to enough susceptible people at the right time. Many get the shot, but not everyone was going to get the disease; some have natural immunity and others are never exposed. Conversely, the shot causes side-effects for some people but not others. Some side-effects are minor, others fatal. The benefits and the risks of the shot are unevenly distributed. Individual people win or lose. The public health question is whether there are more winners than losers.
The public health style of decision-making is, therefore, an organizational activity about the public and affecting the public, but not necessarily involving the public. Public health ethics are therefore quite different from medical ethics, focusing on:
INTERDEPENDENCE, balancing the health of the community with individual rights, recognizing that the health of some often depends on the health of others.
DEVELOPING AND MAINTAINING COMMUNITY TRUST through communication, collaboration, transparency, keeping confidentiality as appropriate, and (ideally) seeking the community’s consent for interventions.
FUNDAMENTALITY, concentrating on the underlying causes of disease as well as the physical and social requirements for healthy communities.
JUSTICE, meaning that public health measures are fairly imposed across the entire population.
Public health is about the common good. It’s not about you, beyond the fact that you are a member of society.
You, as an individual, won’t be making decisions about things that affect you personally; you’ll be told what to do, as you were with all those Covid restrictions and vaccine mandates. This might make sense at the population level, but you don’t benefit when the life saved (or extended) isn’t yours, and you may suffer the harm of a severe adverse reaction to the vaccine.
At its worst, the public health model is paternalistic, “abstract”, and impersonal! Societal problems, societal values, societal decisions, societal consequences, but also your consequences (good or bad). In the end, society will judge whether it was worth the cost, financial and otherwise.6 You might just be collateral damage.
The middle ground
So, at the one extreme we have you making decisions about your own health, based on what matters to you, and at the other extreme we have experts making decisions about you for the greater good, based on abstractions.
In between those two extremes there are various shades of gray. I’ll talk about a couple.
Statistics applied to discrete groups: Cancer X and the Post-MI scenario
First, consider a hypothetical condition, Cancer X.7 For 80% of people with Cancer X, surgery itself is curative, meaning they’ll have no recurrence. The other 20% do well initially but will have a recurrence at some later date, and it could be either treatable or fatal. Post-operative chemotherapy reduces the risk of recurrence by 50%, which means that only 10% will have a recurrence. That sounds pretty good!
Next, imagine 10 patients who have just completed surgery for Cancer X. All ten benefitted from the surgery. We don’t know ahead of time which of them will have a recurrence, so we give chemotherapy to all 10 patients, and then wait for years to see how they fare. As predicted, only one has a recurrence. However:
eight of them didn’t really benefit from the chemo, because they were never destined to have a recurrence.
another one didn’t benefit, because they got the chemo and still had the recurrence.
only one patient actually benefitted from the chemo, the one who was going to have a recurrence but didn’t, and we’ll never know which one that was.
So, ten people got chemo, but only one benefitted. You treat 10 people to benefit one (the ‘number needed to treat’, or NNT, in this case is 10). On the other hand, all ten were harmed, having suffered the inconvenience, side-effects and complications of chemotherapy.
For you, as an individual patient in this scenario, you are making decisions about your own chemotherapy based on what has been shown to work for a group of people, where it might or might not work for you. The one-in-ten odds of benefitting sound good, but the 100% chance of nasty chemo side-effects isn’t appealing. This kind of decision-making is hard8. While the cancer specialists, looking at it through the greater good lens, might see it as a ‘no-brainer’, your decision reflects what’s important to you, balancing off abstract possible future benefits against concrete immediate nasty risks. Effectively, you’re buying a lottery ticket with a 1-in-10 chance of winning something (no cancer recurrence) years from now, paying for it with near-term suffering and risk. Even worse, if you were the one who was going to have a recurrence but didn’t, your outcome (no recurrence) is no different from the other eight who were never going to have a recurrence. Practically speaking, you won’t actually know that you won! With all the facts in front of them, some people buy the ticket, others don’t.9
So, it’s a hybrid model, somewhere in between the public health and medical care models. You and others with cancer like yours are in a group, separate from everybody else. You’ve each benefitted from the surgery, the decision you each face now is about chemotherapy. At a group level, the benefits outweigh the risks, but not necessarily at the individual level. Nobody should be telling you what to do. The decision is yours to make.
As a doctor advising a patient about chemotherapy in this scenario, the ethical principles of medical care should apply. Patients have freedom of choice, and that choice should be informed, but it can be difficult to explain how the potential risks and harms weigh up against the benefits. Chemo is certainly harmful; few people go through it without consequences. The question is whether there’s a benefit. We don’t see each patient benefitting by 10%. We have 9 patients with 0% benefit and one patient with 100% benefit. Is a 1-in-10 chance of no recurrence an equal benefit for all ten patients?10
I worry that the decision-making in these cases isn’t always as shared as it should be. Ideally, the post-op chemo decision should be made by the patient, under the shared decision-making model, where the physician provides information about the range of options, the patient expresses his or her values and preferences, and together they arrive at the decision that’s best for this patient at this time. My theory is that sometimes the post-op chemo is presented as just another component of the treatment plan (like the bumper is part of the car), perhaps framing it up as “completing the course of treatment”. This leaves patients who decline chemo thinking that they’ve been incompletely treated or feeling like they are fighting against medical pressure.11
There are plenty of similar situations in medicine. As another example, following a heart attack (myocardial infarction), it’s recommended that patients take statins (drugs which lower the cholesterol) to reduce the risk of further myocardial infarctions, strokes, or death. As with the Cancer X example, these patients have benefitted from their initial treatment and are now facing a separate decision about their ongoing care. The drugs do reduce the risk, but the 5-year NNT (number needed to treat) is 29, meaning that you’ll have to feed daily statins to 29 patients for 5 years so that one will benefit. Are patients are being given this information, with the option to make their own decisions? I suspect the prescription is more often presented to the patient as being necessary to prevent another heart attack, a stroke, or even death. In other words, an offer you don’t want to refuse.12
Statistics run amok, the Hypertension scenario
When it comes to deciding about treatment, you might think that hypertension is just like Cancer X. You have a disease and are making decisions about treating your own hypertension based on what works on average for a group of people.
However, with hypertension, there’s an important difference in how the disease itself is defined.
With Cancer X, you either have the disease or you don’t, based on the pathological examination of your tissues. In hypertension, there’s really little or nothing to see, other than your blood pressure measurement. There are usually no symptoms and there’s no abnormal pathology. It’s basically just a matter of statistics. Let me explain.
If you round up a few thousand people and check their blood pressure a few times, averaging the readings for each individual, you’ll get a range of readings clustered around the average in the classic Bell curve distribution.
This sort of pattern is seen for many, if not all, physiological parameters, including height, weight, blood chemistry, etc. In such cases, the usual approach is to define people in the middle 95% of the curve as “normal” and the 2.5% outliers at either end as “abnormal”.
For blood pressure, however, various expert groupings (of which there are many) have set the outlier threshold differently, based on their assessment of risks. They literally vote on it! This is classic public health thinking. You look at the entire population, find the “at risk group”, and then tell them what to do, for the greater good. Because everybody is at risk, and the risk is lower if the blood pressure is lowered, they make the case for treating everyone.
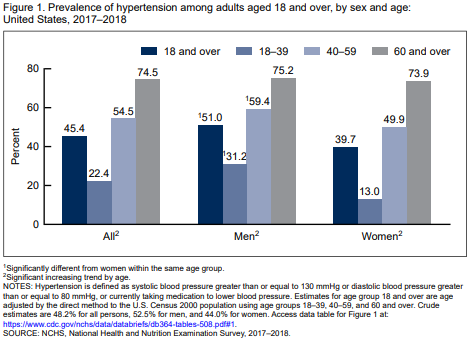
Unsurprisingly, the diagnosis of hypertension is now extremely common.
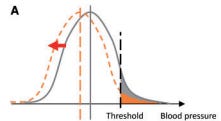
Yes, you read that right! If you diagnose high blood pressure as being a blood pressure greater than 130/80, then, in 2017-18, 45.4% of Americans aged 18 and over were hypertensive, rising to 74.5% of those 60 and over! The implication is that every second person would benefit by having their blood pressure lowered.13 Some public health folks now go even further, suggesting that everyone should have their blood pressure lowered, shown on the bell curve picture above as moving the entire curve to the left.14
For you, higher blood pressure doesn’t make you sick, it just increases your future risk of heart attacks, strokes, death, etc. Realistically, we are all at risk for bad things happening, and some people have a higher risk than others. We know about risks by studying what happens to groups of people with similar blood pressures. There’s no blood pressure at which you are guaranteed to have a stroke or heart attack, and there’s no magic number above which your risk takes a huge jump. There’s just a gradual increase in your risk as your blood pressure rises. Your blood pressure could be high and you live to be 100, or your blood pressure could be normal and you die of a stroke at age 40.
Complicating matters further, your blood pressure is only one risk factor for heart attacks, etc. There are many others, including your age, sex, family history, cholesterol levels, weight, and other diseases (like diabetes). Some can be changed, others can’t.15
If you approach this at the individual level, in the medical care paradigm, your best approach is shared decision-making. Your physician provides information about your blood pressure (and other risk factors), the level of risk that you face, and the range of treatment options. You consider your values and preferences. Together you arrive at the plan that’s best for you at this time. Reducing your blood pressure reduces your risk, but the amount by which the risk is reduced depends on how high your blood pressure is in the first place, and your other risk factors. If your blood pressure is less than 160/100 and you are otherwise well, you gain nothing (in terms of risk reduction) by lowering your blood pressure with medication. If it’s higher, treatment lowers your risk more, but we still have to treat you and dozens of people like you for years on end to prevent a single death. The NNT is quite high.
As with Cancer X, the benefits and the risks of treatment are unevenly distributed. Anti-hypertensive drugs cost money and have side-effects, so they are “harmful”. The benefit is unclear; treatment may or may not affect your outcome. While some people benefit, we never know which ones. It’s just another lottery!
Public health thinking says what matters is that there are more winners than losers.
However, if 50% of the population have hypertension, that leads to millions of complicated individual shared care conversations. In this case, it’s not just a conversation about your odds of benefitting from or being harmed by treatment, it’s a conversation about the fact that the diagnosis itself is based entirely on statistics about risk. As with post-op chemo for Cancer X, my hypothesis is that doctors cut corners, telling anyone with high readings that they have a disease, hypertension, and that makes treatment seem necessary, less a matter of personal choice. “You have hypertension, and treatment reduces your risk of heart attacks, strokes, and death. No, there’s no immediate benefit to lowering your blood pressure, but we’ll focus on getting the numbers lower”. Any benefit lies in reducing future risk, but you probably have no idea what your baseline risk is, or how much it will be reduced. You could take drugs for years with no personal benefit, or you could be the one who has a heart attack or stroke despite having taken medication. Meanwhile, you buy drugs, take them, suffer their side-effects, and see yourself as having an illness.16
So, this is another hybrid model, but much closer to the public health model. You and others with blood pressure like yours form an ill-defined group, with nothing to separate you from everybody else except statistical variation. Is it right to pretend that the rationale for treatment and the ethical framework are the ones that apply in the medical care model?
In conclusion…
The “medical care model” and the “public health model” sit at opposite ends of a spectrum, like this:
Towards the left, the public health model dominates, defining problems and their solutions based on statistical risks and mathematical models. Towards the right, decision-making reflects what’s best for the individual patient. The guiding ethical frameworks differ at the two extremes.
It’s unclear how those different and sometimes conflicting ethical principles apply in the middle, where patients and their health care providers strive to make informed shared decisions about their health. In particular, decisions about future risks often involve complex public health-style logic but are often misleadingly framed up as simple medical care decisions.
In the next post, I’ll look at how this applies to breast cancer screening.
Of note, even though somebody else seems to be paying the bill, in the end it’s you. You can pay directly, you can pay through insurance premiums, you can pay through working for an employer who pays the premiums, or you can pay taxes so that the government can pay for your healthcare. Health care is never “free”!
If you are 20 and otherwise healthy, the surgical option might be the obvious choice. If you are 95 with end-stage lung cancer and one week to live, you might decide to forego the appendectomy.
Most public health interventions affect communities and institutions (i.e. hospitals, schools, restaurants, etc.).
Their scope has since broadened to health promotion and the prevention of diseases related to lifestyle, like smoking and obesity. Some would like them to go further, by aiming to dismantle racism, social and economic inequities, and other forms of oppression.
You’ll know that you are in public health territory when you (or your healthcare provider) start talking about probabilities, ‘statistical lives’ saved, ‘deaths avoided’, or ‘quality-adjusted life years’ added, while some harms are accepted as an ‘acceptable cost’ of doing business.
Many argue that the Covid response showed public health decision-making at its worst. Interestingly, there’s been precious little effort since to assess whether the societal benefits of the Covid response outweighed the harms.
While Cancer X is hypothetical, this scenario not unlike what you see with several different types of cancer.
There’s plenty of research showing that people have a very hard time balancing present costs and future benefits. Among other things, there’s a tendency to exaggerate the risk of good outcomes (like winning the lottery) and bad outcomes (like death).
We’ve had two recent examples in the news. Princess Kate had some unspecified form of cancer and underwent a course of “preventive chemotherapy”. It seems reasonably clear that she had a choice about it, and she chose to proceed. Elle MacPherson, on the other hand, had breast cancer surgery and “refused” the subsequent chemotherapy, making the claim that her “intuitive, heart-led, holistic” approach explains her lack of recurrence thus far. For both of them, there’s a chance that the surgery was curative, and the chemo was unnecessary. There’s also a chance that either one could have a future recurrence.
Is a lottery ticket a benefit? Some people place a value on hope, and they would say that it is a good use of their money. Others feel disappointed every time they don’t win, and so they see lottery tickets as a poor use of their money. Sure, I’ll take a free lottery ticket, because it comes at no cost to me, but I wouldn’t pay for the lottery ticket with my own money. The challenge with health care is that it seems “free”, which further distorts people’s thinking. Are you more likely to have chemotherapy, knowing it’s unlikely to help, when you aren’t paying for it? It seems ungrateful to turn down something that’s free and might be helpful.
Reading between the lines of the Elle MacPherson situation, I wonder if this isn’t what was going on.
Going further, it’s increasingly common that health record systems are being built to issue care prompts, such that doctors seeing “eligible patients” (those who have had a heart attack) will be “prompted” to prescribe statins. In some cases, those who don’t obey the prompts are penalized for failing to provide “evidence-based care”.
This should come as no great surprise. They are saying that anyone with “above average risk” should be diagnosed with hypertension and offered treatment. By definition, half the population has “above average risk”! The other half are below average, but still have a measurable risk, which could be reduced further.
At this point, you have to wonder whether the prescribed interventions should be societal, rather than individual. For example, since blood pressure and other cardiac risk factors are heavily influenced by weight, and there are so many overweight people, perhaps public health should address the root causes of obesity (the food supply, perhaps?), rather than having individual doctors working with individual patients to devise individual treatment plans. It would fit with the public health principle of fundamentality, concentrating on the underlying causes of disease as well as the physical and social requirements for healthy communities
No, changing to your preferred gender won’t alter your risk!
Age is the biggest risk factor for a lot of things. I used to tell my patients that they could reduce their risk of many things if they could stop aging. Of course, there’s only one way to do that!
There’s evidence that disease labels adversely affect work attendance, employability, insurability, etc.